Hello POCUS people,
We are back with our weekly popular POCUS puzzles with the cases-of-the-week and cases-of-the-geek to share! Be sure to sign up for our COTW emails for them to be delivered straight to your email inbox!
The Case
A 75 year old male presents to the emergency department with delirium and fever. You use your POCUS skills to look for a possible source of infection in his lungs.
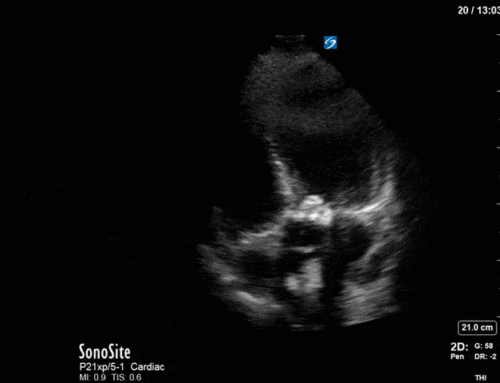
Both sides of the anterior chest showed the following pattern:

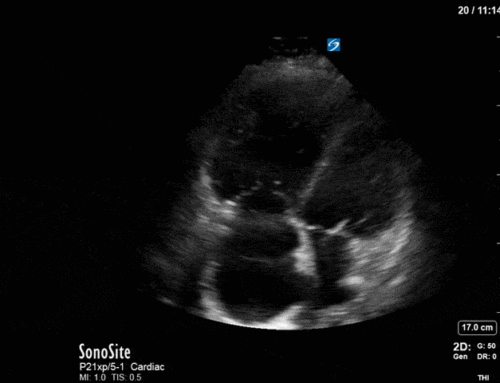
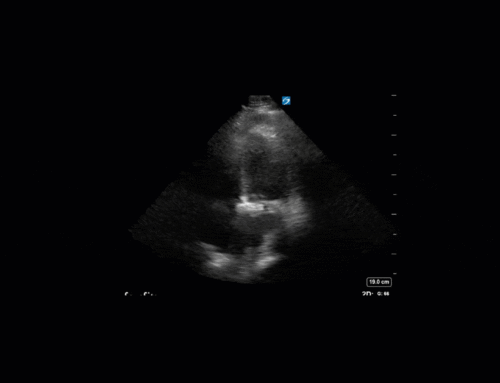
The right base/PLAPS showed:
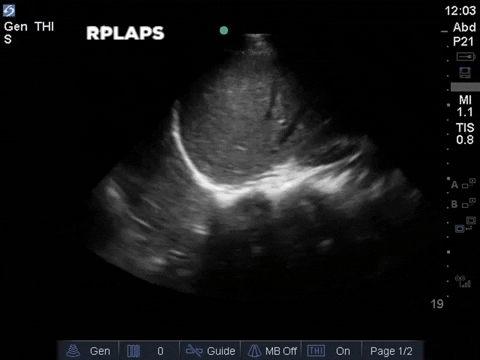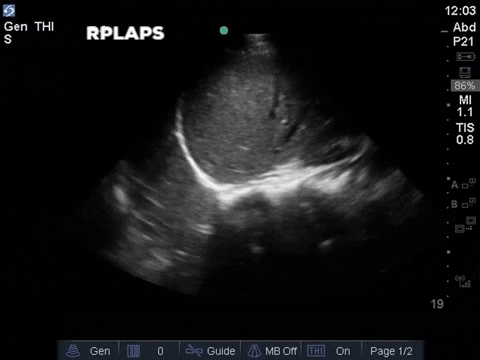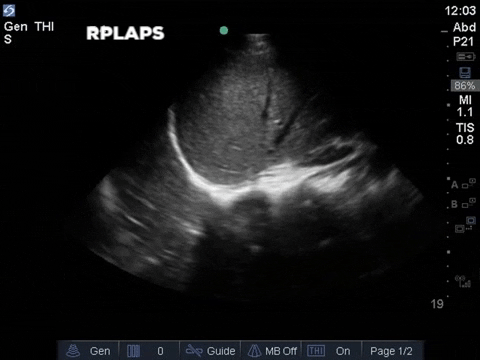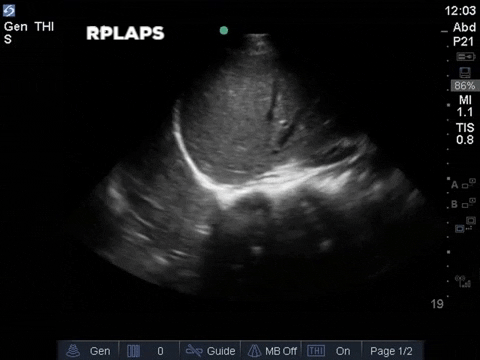
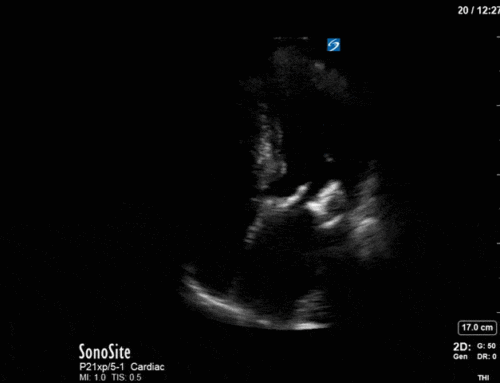
The left base/PLAPS showed:
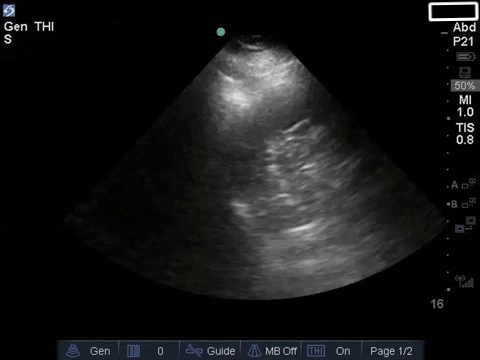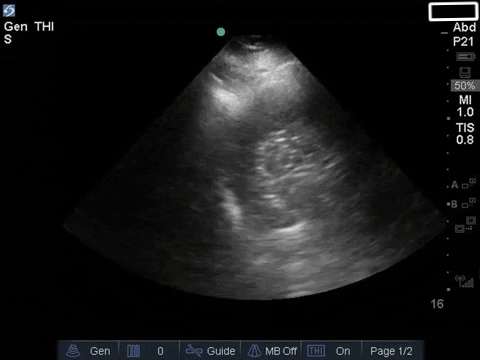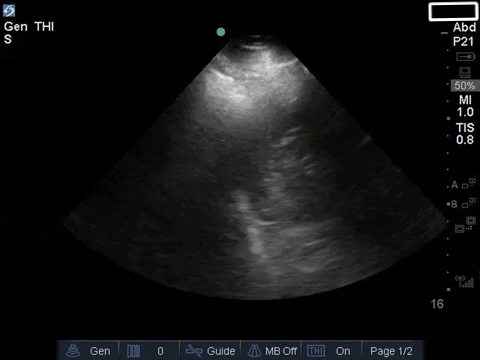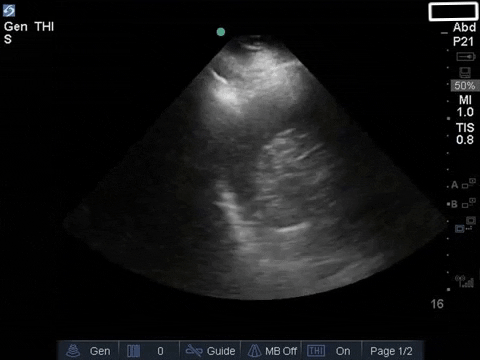
COTG
A 48 year old female admitted to the ICU with severe traumatic brain injury and diffuse axonal injury is treated for raised intracranial pressure with propofol, midazolam, hydromorphone, hypertonic saline and mechanical ventilation. An ICP monitor is inserted and over the first 36 hours her ICP remains <20mm Hg with the medical therapy. Over the following 2 hours the patient has an increase in ICP >50mm Hg which is refractory to aggressive medical therapy. A point-of-care transcranial doppler is conducted and shows the following (similar findings bilaterally):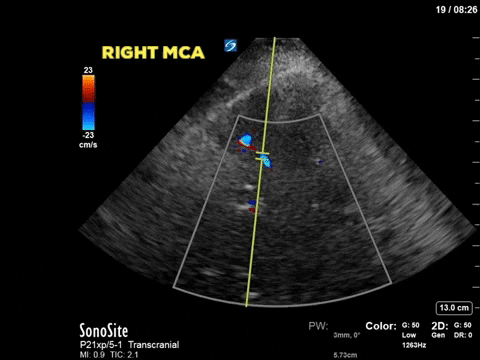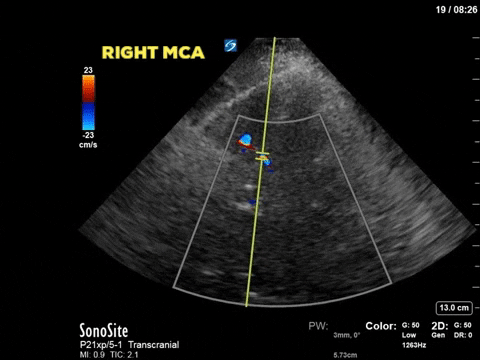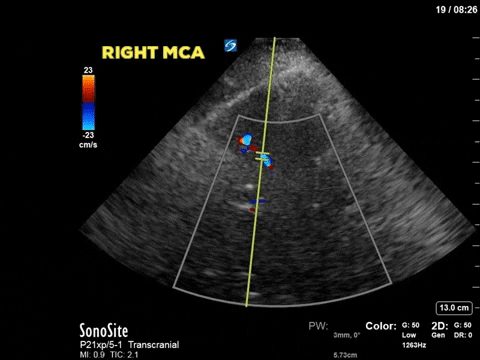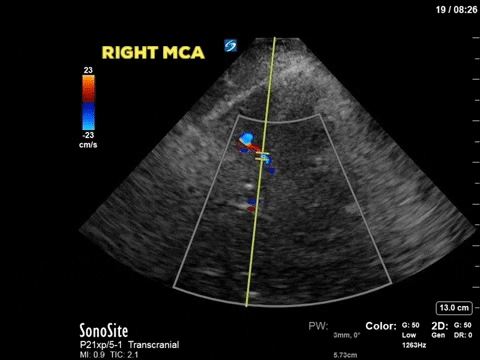
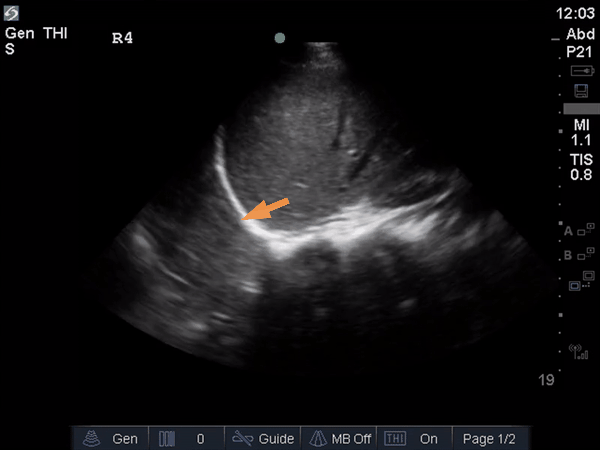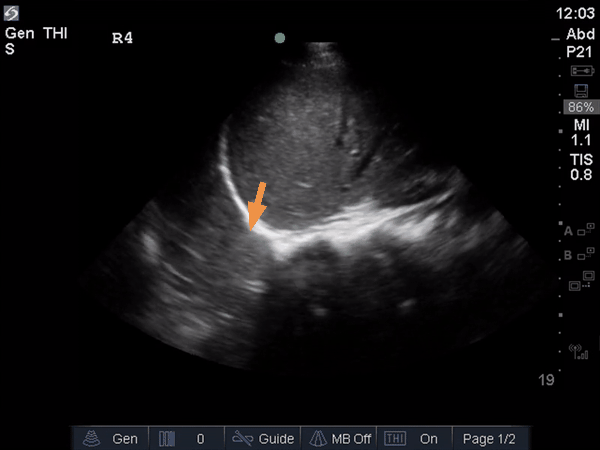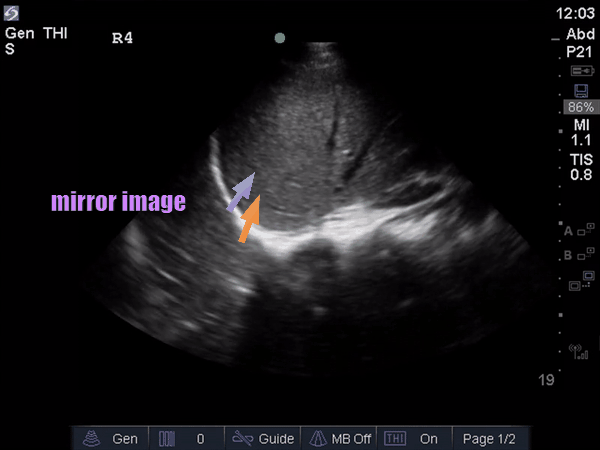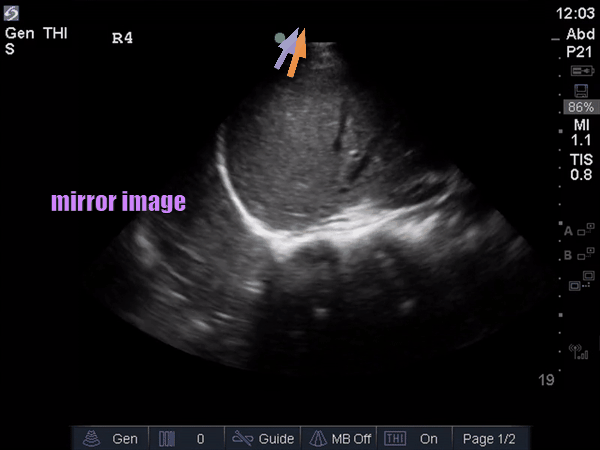
The anterior chest revealed an A line pattern with lung sliding indicating a well aerated lung with no evidence of a pneumothorax in this area. The left base, although it was a suboptimal view, showed a curtain sign and no consolidation or pleural effusion. The right base is worth discussing a bit! There appears to be an isoechoic structure above the right hemidiaphragm which looks a lot like lung hepatization but in fact this is a mirror image artifact. The clip below shows the true path of the ultrasound beam (orange arrow) and the “apparent path” (purple arrow) as interpreted by the ultrasound machine. The ultrasound machine assumes that the beam travels in a straight line contacts tissue structures, reflects and travels back towards the ultrasound transducer. This is of course not true, due to reflection and refraction phenomena. The diaphragm and pericardium are common sites of mirror-image artifact because of their highly reflective tissue and flat surface. Other than this being a common location for this artifact the second clue to look for is the spine sign. The absence of the spine above the diaphragm suggests that this is not consolidated/hepatized lung tissue. To be sure change the angle of the ultrasound probe or view from a different rib interspace to minimize/avoid the mirror image artifact.
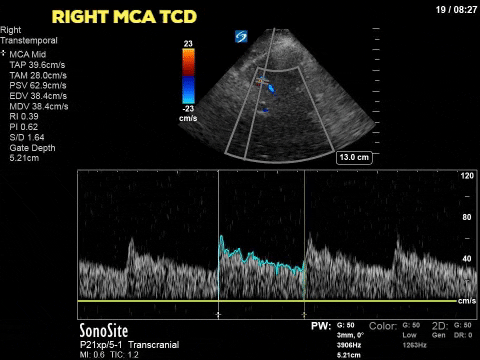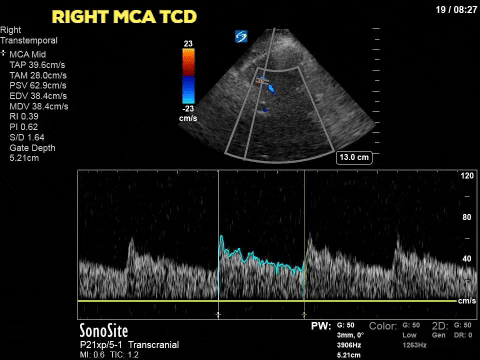
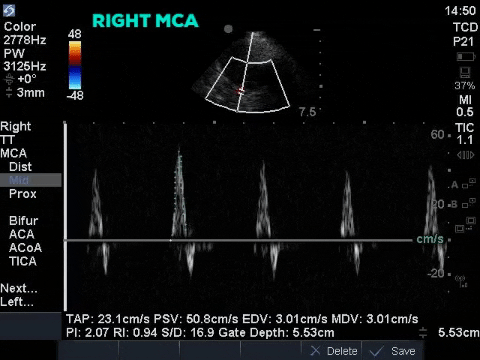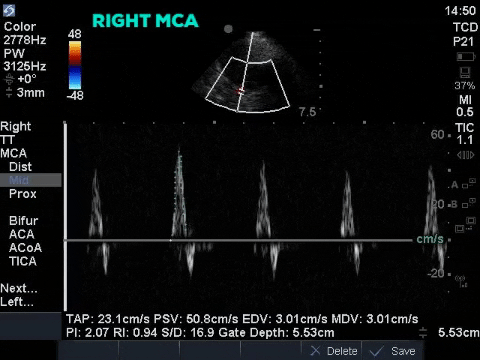
The first image is taken from the transtemporal window and shows the middle cerebral artery with colour doppler and the pulse-wave doppler gate overlying the vessel. The following still image shows the resultant doppler flow pattern. As you can see the doppler flow ranges from 35cm/s to 70cm/s and is always positive, suggesting that blood flow is constant (during systole and diastole) and towards the ultrasound transducer. This is the flow pattern in a normal MCA flow state. By tracing the envelope of one cycle we can obtain the pulsatility index (PI). The PI is a numeric representation of the difference between the systolic and diastolic velocity which tends to increase as ICP increases. Clinically the PI can be used to estimate ICP, as was shown by Bellner at el, 2004. Their study found a correlation coefficient of 0.938 using the following equation ICP = [10.93 X PI] – 1.28. Using this equation our patient’s ICP would be estimated at 5.5mm Hg. Click here for a clinically relevant review of TCD applications for the intensivist. Based on this POCUS study and the incongruent results with the ICP monitor, the patient had a repeat CT scan of the brain which showed a decrease in the generalized brain edema, and less sulcal effacement from the date of admission. As such the ICP monitor was felt to have malfunctioned and was subsequently removed. The image below is the TCD of a patient with multiple strokes, dilated pupils and shows diastolic flow reversal which suggests impending cerebral circulatory arrest.
Thanks and happy scanning!
Marko Balan and the WesternSono POCUS team