Case of the Week: February 14, 2020
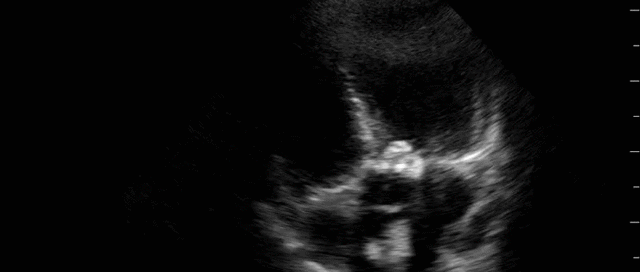
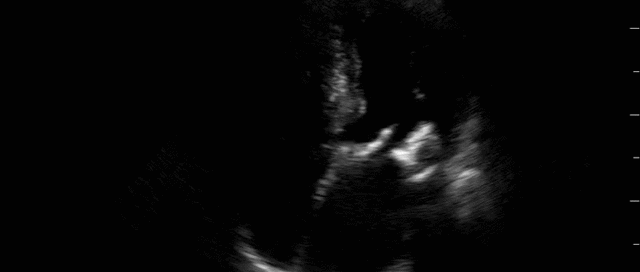
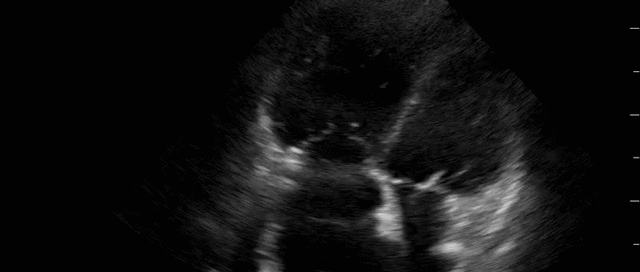
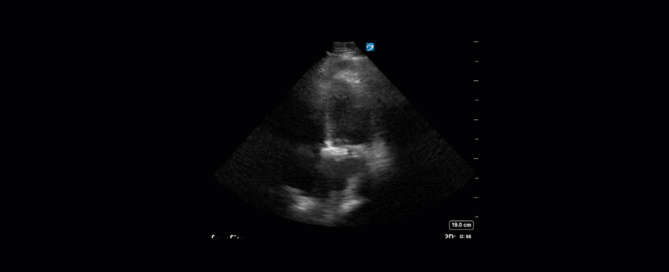
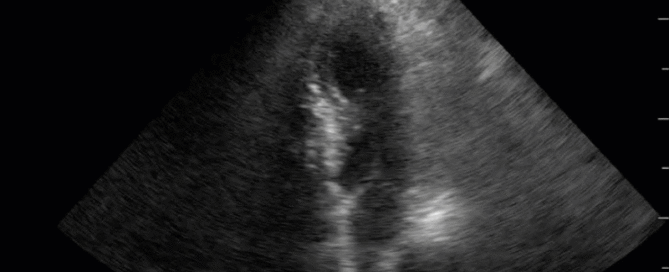
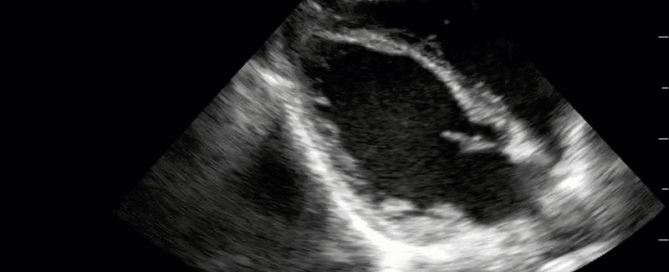
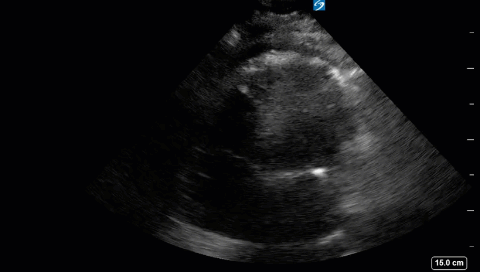
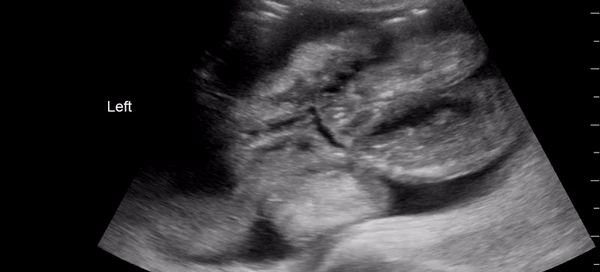
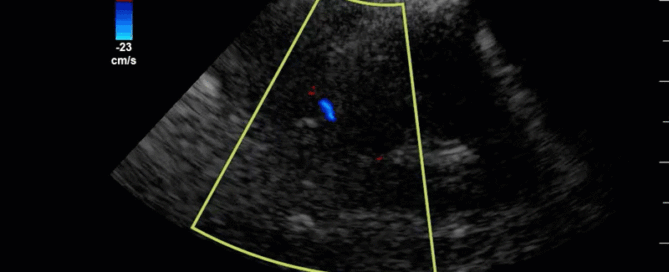
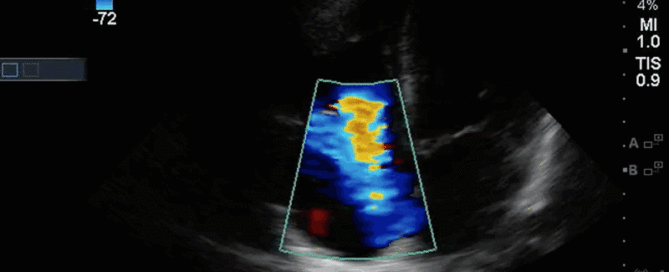
This is a 58yo F with ESRD with a history of known infective endocarditis of her AV for which she had previously completed a prolonged course of IV antibiotics. She was admitted to the ICU for worsening dyspnea. The POCUS team performed cardiac exam with some of the most striking clips shown below. What do you think? What complication of her endocarditis is shown and how would you grade its severity?