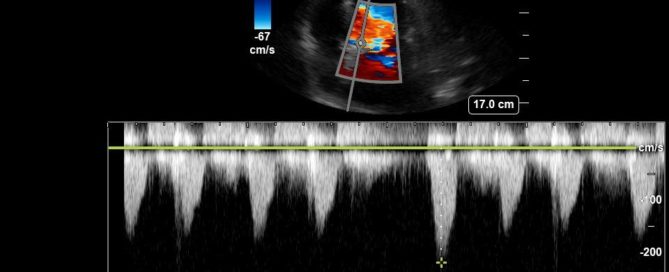
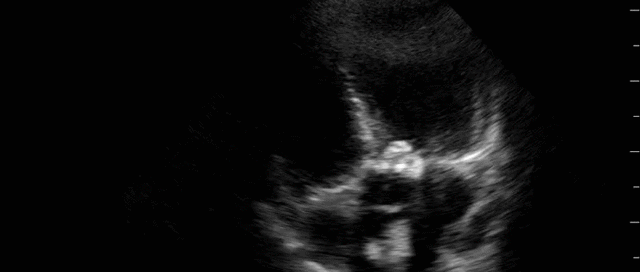
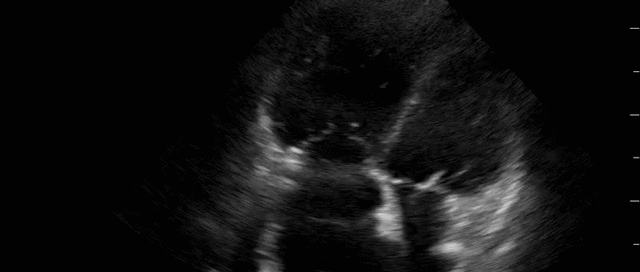
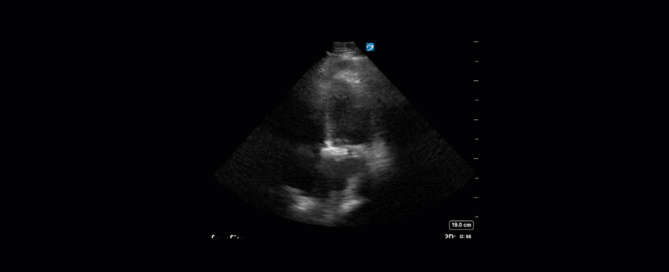
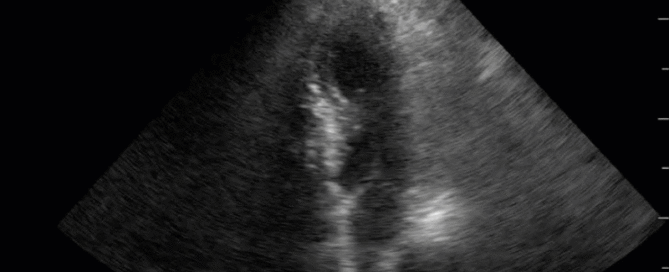
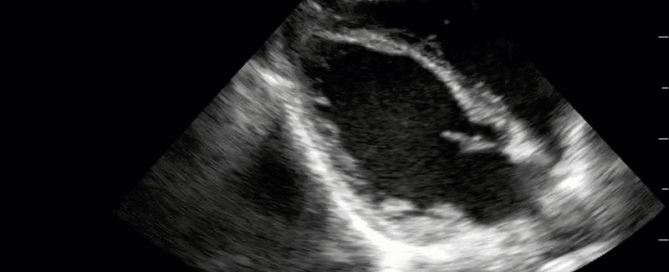
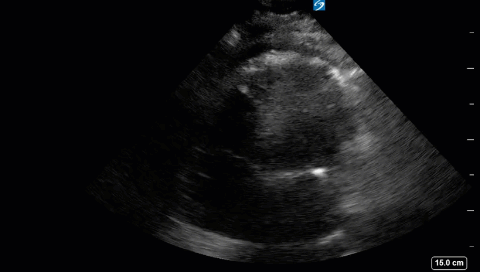
Advanced Critical Care Ultrasound Quantitative Assessment Resource
Our previous Critical Care Ultrasound Fellow, Marko Balan MD FRCPC, who is now an intensivist at Dartmouth General Hospital has put together a comprehensive, point-of-care resource containing a wealth of advanced critical care ultrasound material. You will find in it extensive coverage of quantitative techniques that can be used for the assessment of the critically ill. Topics include: hemodynamic assessment, diastology, valvular assessment, pericardial assessment, [...]