Hi POCUS enthusiasts,
Happy new year! Based on feedback from a few of our die-hard POCUS people (namely Dr Rob Leeper), for 2019 we will be introducing a new and exciting element to our COTW/COTG: participant interactivity and collaboration! After this week, we will be hosting the COTW/COTG on the westernsono website where participants will be encouraged to post their answers and vote on the answers submitted by others. Go to westernsono.ca and sign up in the box on the right side of the page. You will receive an email asking for final confirmation – then you’re ready to submit and engage!
The Case
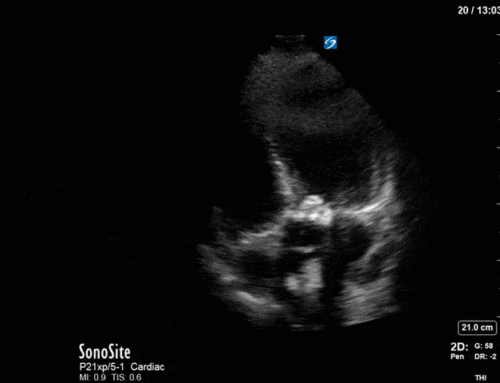
A middle aged man presented to the Emergency Department 5 days after a ERCP and stent insertion for obstructive jaundice feeling unwell, feverish, and lightheaded. He rapidly deteriorated with hypotension and was admitted to the ICU with sepsis NYD. 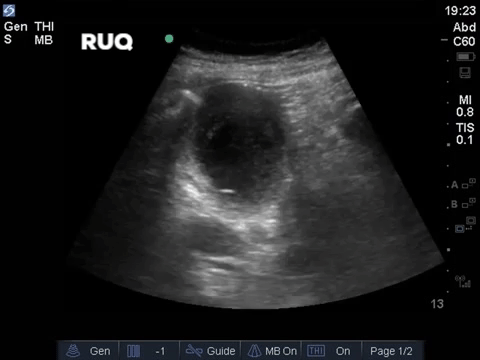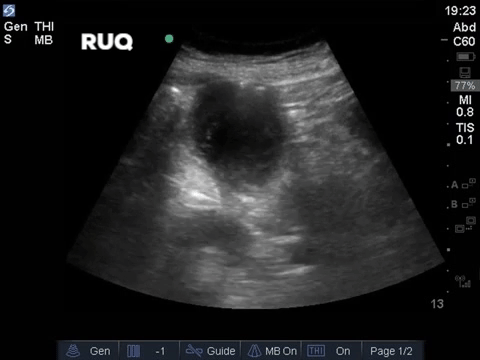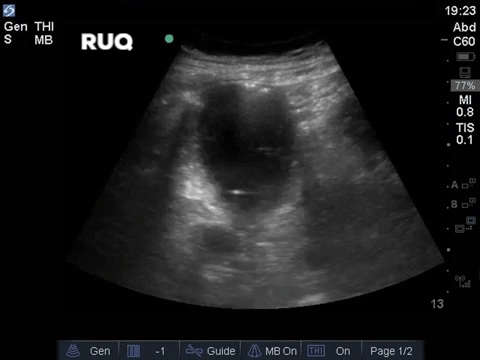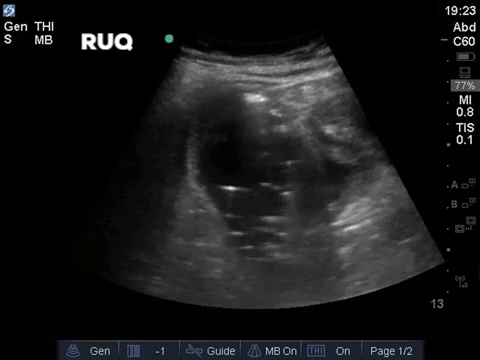
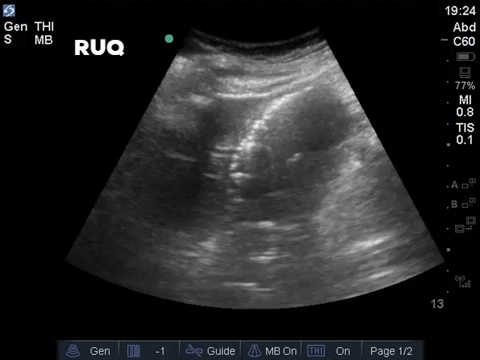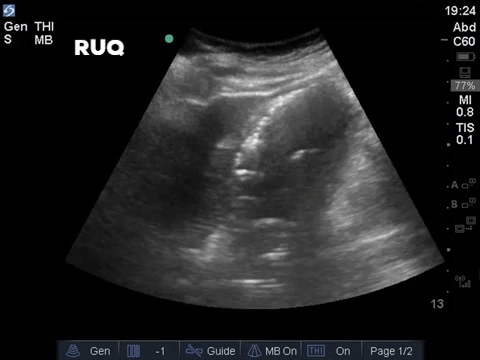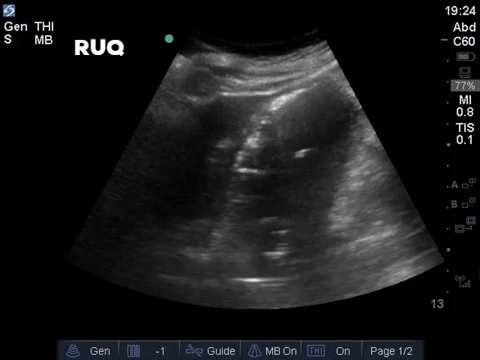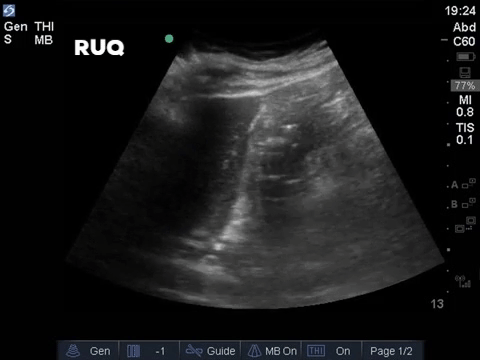
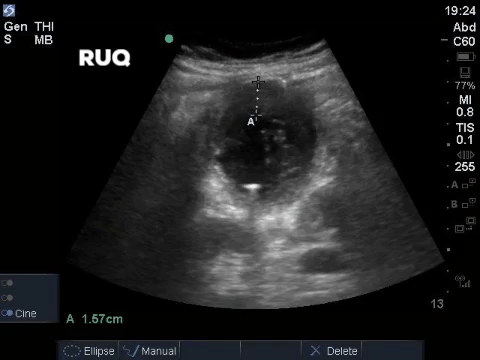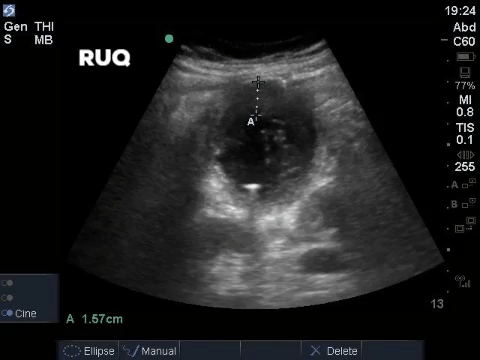
COTG
Let’s cut right to the chase with this one, since the answer to last week’s COTG might feel a bit painful.
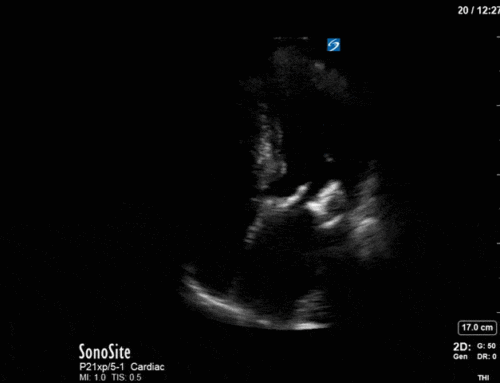
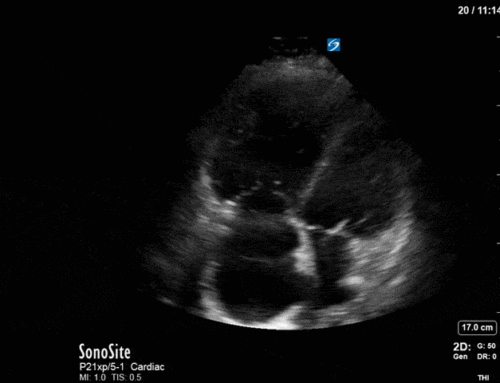
A 32 year old male cyclist vs vehicle trauma patient is hypotensive in the trauma bay. The junior resident shows you these clips and is gearing up for bilateral chest tube insertion.
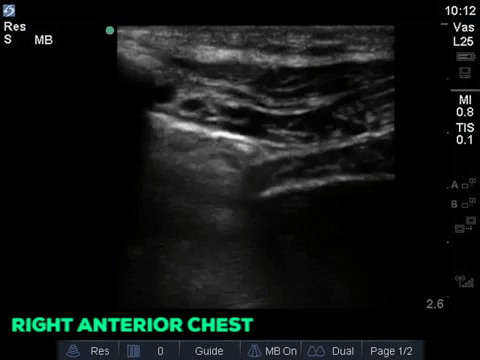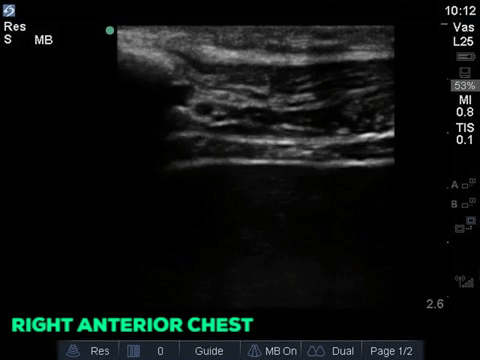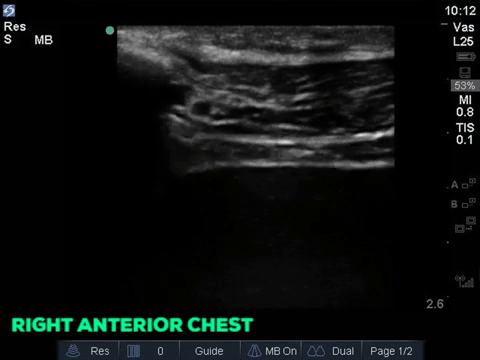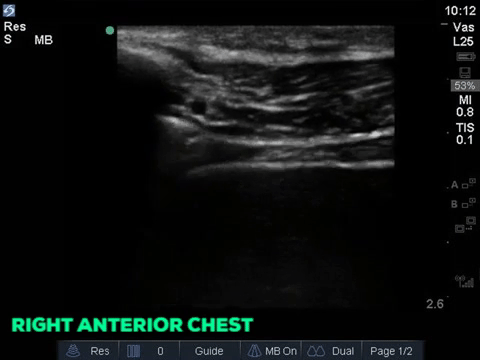
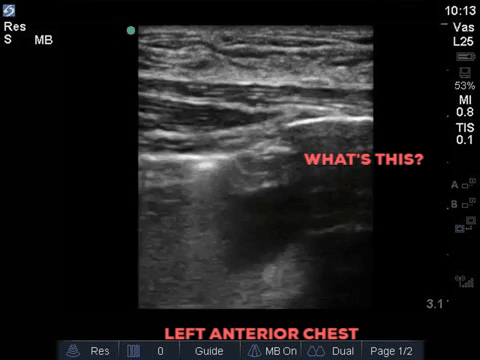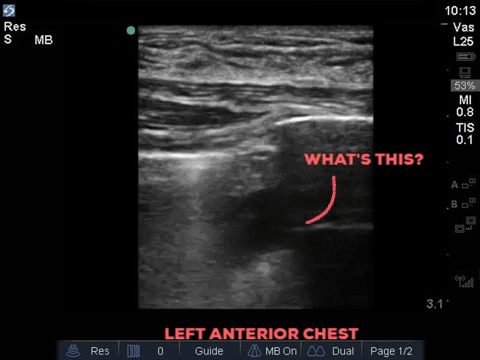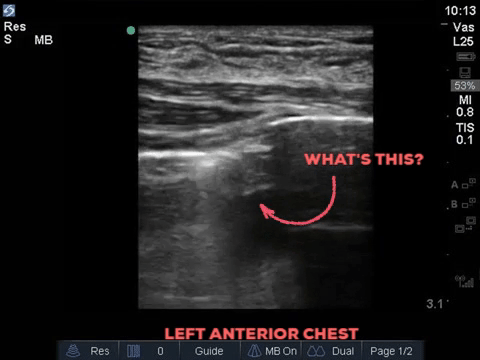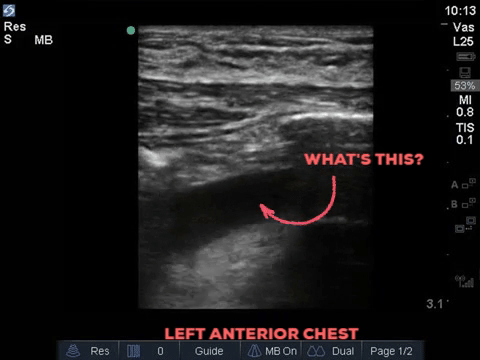
Answer to Last Weeks Case
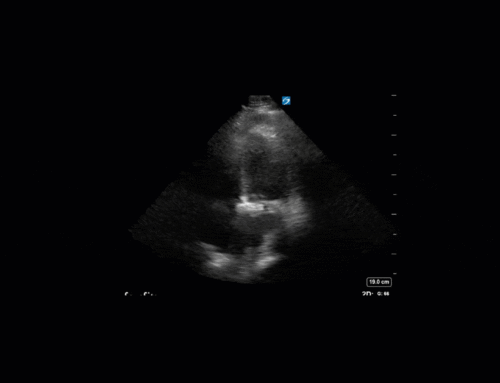
A 62 year-old female was admitted to the ICU after a presumed hypoxic cardiac arrest. She had a history of “heart failure” and renal failure on dialysis. Based on these two views alone, what kind of “congestive heart failure” does she appear have? What common post-arrest intervention causes the heart rate we are seeing?
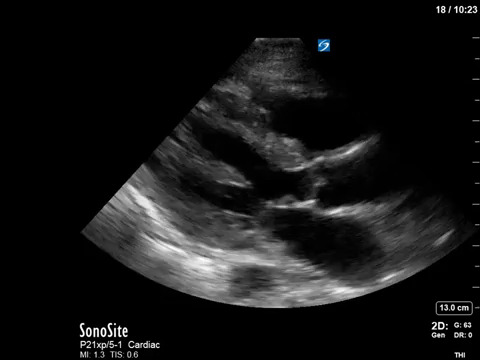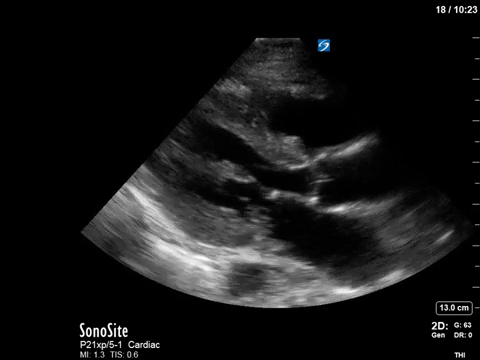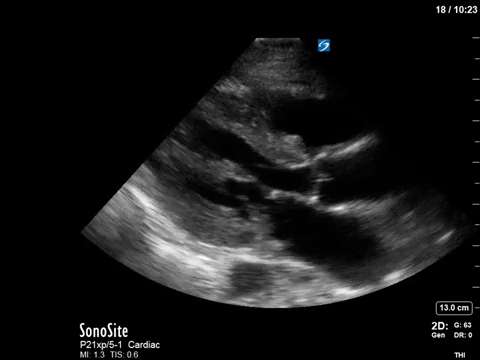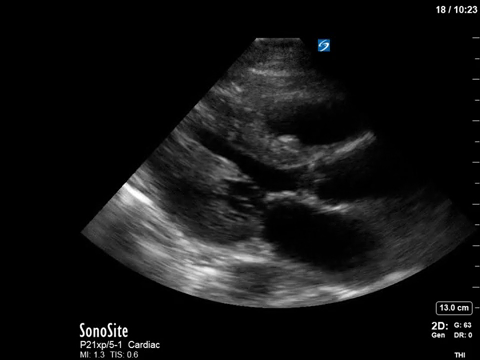
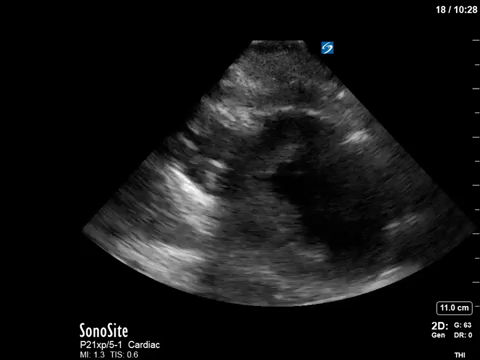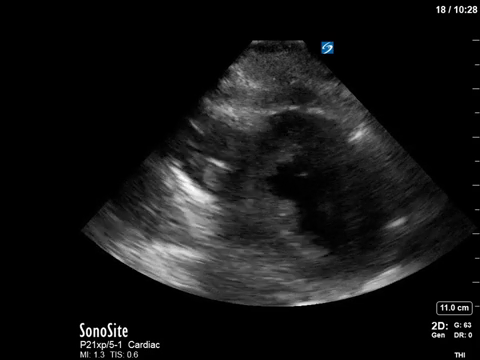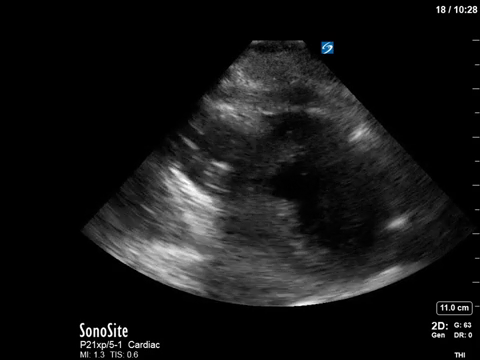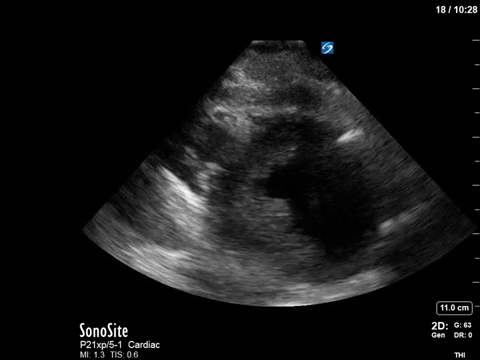
In terms of the “heart failure”, on first look the heart looks….sluuuuuggish, but have another look. On careful evaluation we see the myocardial excursion and thickening is actually pretty good, it’s just slooooow (i.e. bradycardic), which as all of you would know, can sometimes fool the novice POCUS practitioner into thinking that the systolic function is actually depressed. What this patient had was heart failure with preserved ejection fraction, or HFpEF, or HeffPeff, or diastolic dysfunction or diastolic heart failure (or whatever else you might want to call it!). Oh yes, and the bradycardia was in fact a result of the therapeutic hypothermia in this post cardiac arrest patient.
Answer to Last Weeks COTG
Below is some advanced POCUS applications in the same patient to supplement your above hypothesis. What do these still images tell us about the patient’s heart function and pressures?
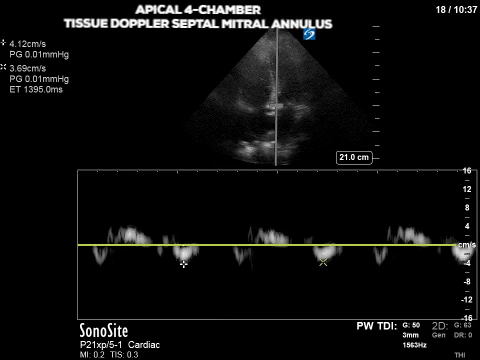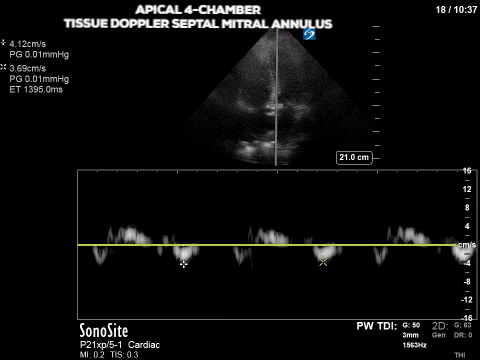
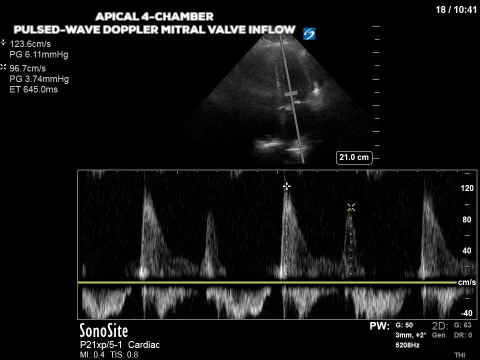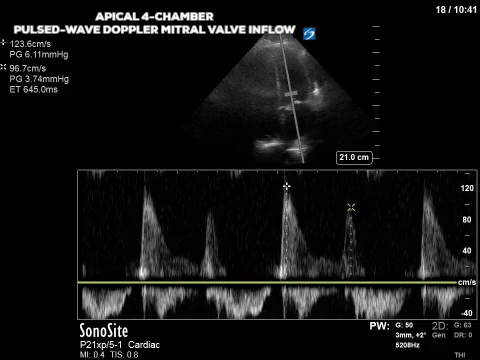
The final image assesses the mitral valve inflow velocity and here we have measured the peak velocity of two of the four phases of the diastolic period. The E wave (think early wave) occurs first and is the initial gush of blood from the LA to the LV; it measures 123.6cm/s. The second peak, called the A wave (think “atrial kick”) is 96.7cm/s. Although in some patients the E/A relationship in and of itself can suggest diastolic dysfunction in many it can’t be used as a standalone measure. Furthermore E wave is affected by volume status or preload in addition to a multitude of other factors (heart rhythm, mitral valve function etc). We can get around the effect of preload on the E wave by finding another measure that is considered preload independent. The velocity of the mitral annulus during diastole is considered as such a measure; the slower the mitral annulus moves away from the apex during diastole, the slower the LV relaxation which relates to diastolic dysfunction.
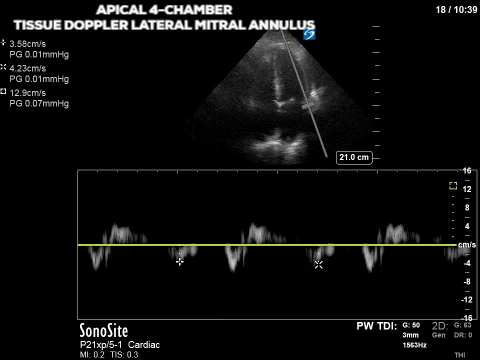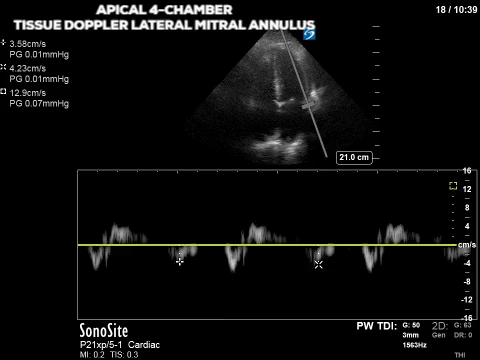
The first two images show an apical four-chamber view with the pulsed-wave tissue doppler set at the septal and lateral mitral annulus (sometimes referred to as septal e’ and lat e’, respectively). As with other applications of PW doppler, tissue doppler measures the velocity of movement within the gate but is optimized for the typical velocity range of myocardial tissue. From the ASE guidelines, lateral e’ <10 and septal e’ <7 are some of the criteria for diastolic dysfunction. So our patient’s tissue doppler velocities of ~4cm/s are definitely consistent with diastolic dysfunction.
There’s so much more to say but I think I’ve already geeked out enough for one week. Attached is a paper by Greenstein & Mayo proposing a simplified approach to assessment of diastolic dysfunction in patients in the ICU. Greenstein and Mayo 2018
Happy scanning,
The POCUS Team