Hi everyone. It’s Matt back today, so you’ll have wait until next week for more EyeScandy!
The Case
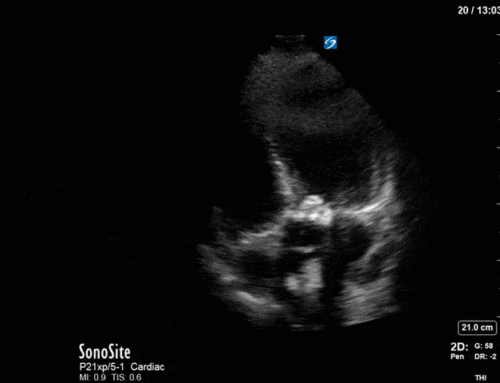
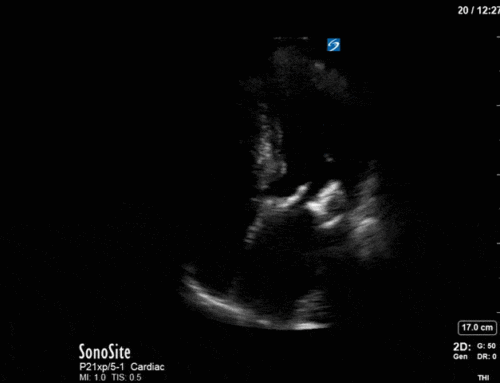
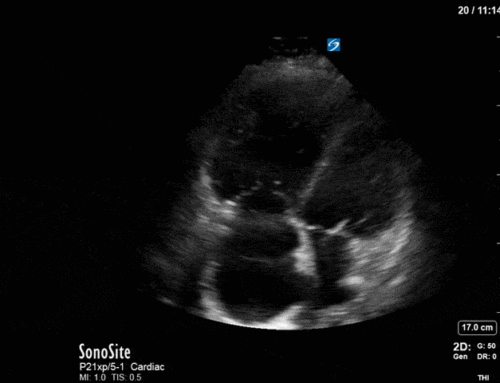
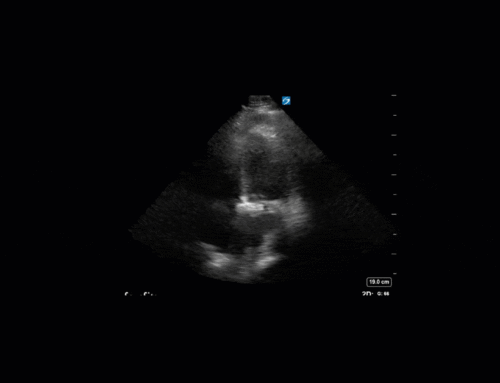
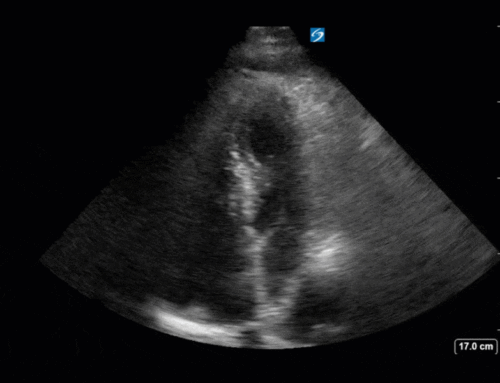
This is a case of a 56 yo F admitted with sepsis and MSSA bacteremia. A CT Head revealed several lesions concerning for septic emboli. She had known chronic significant mitral valve pathology documented prior to her admission. The POCUS team keen to see this pathology and to look for any additional signs of infective endocarditis. What do you notice about the valve on the 2D echo images and what specifically do you see on its colour doppler interrogation?
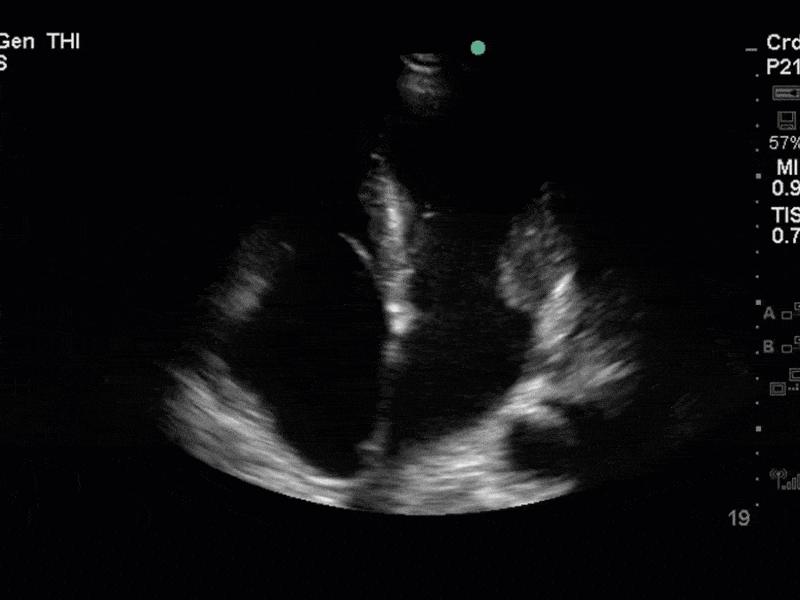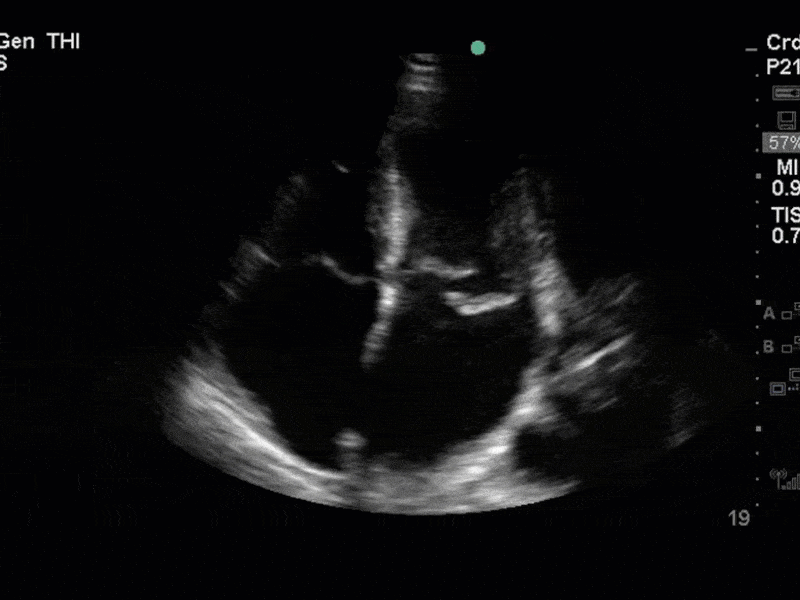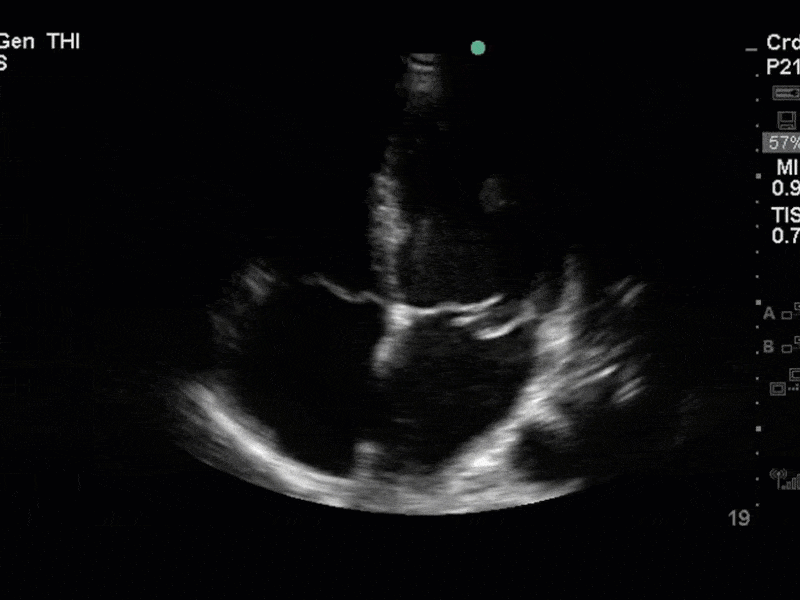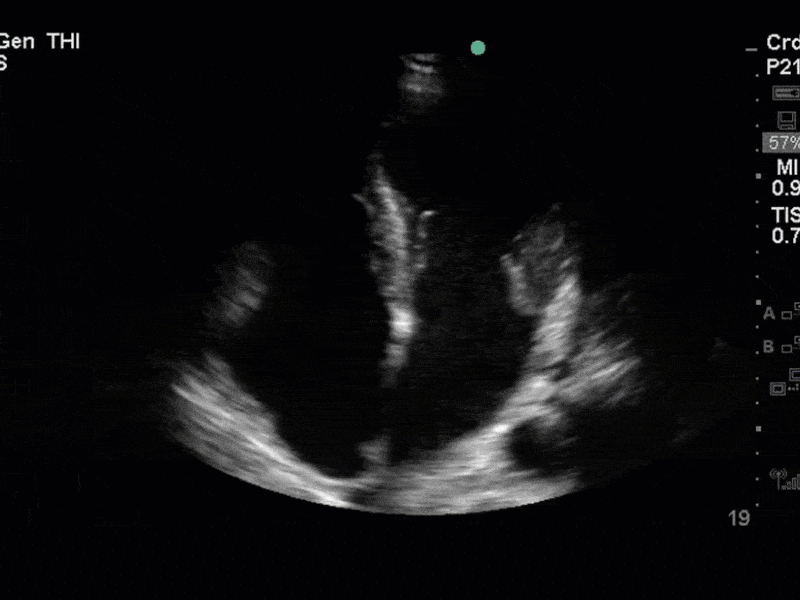
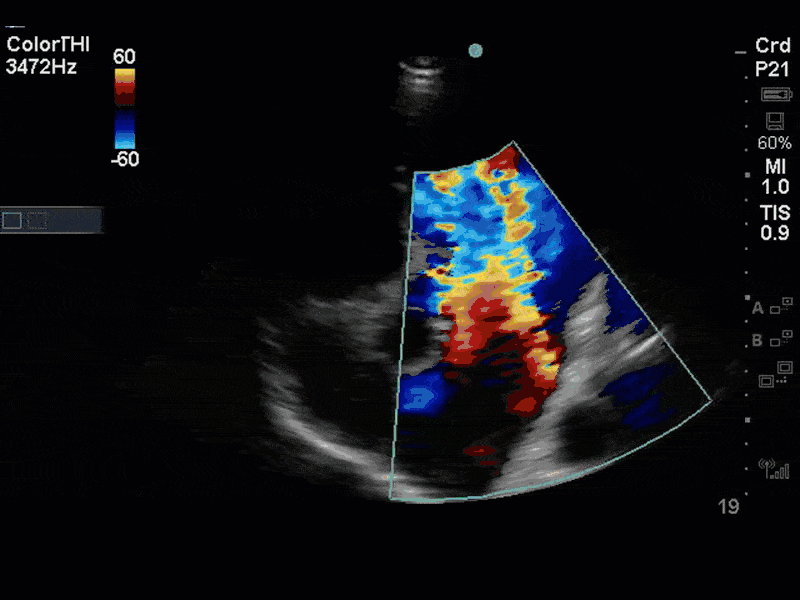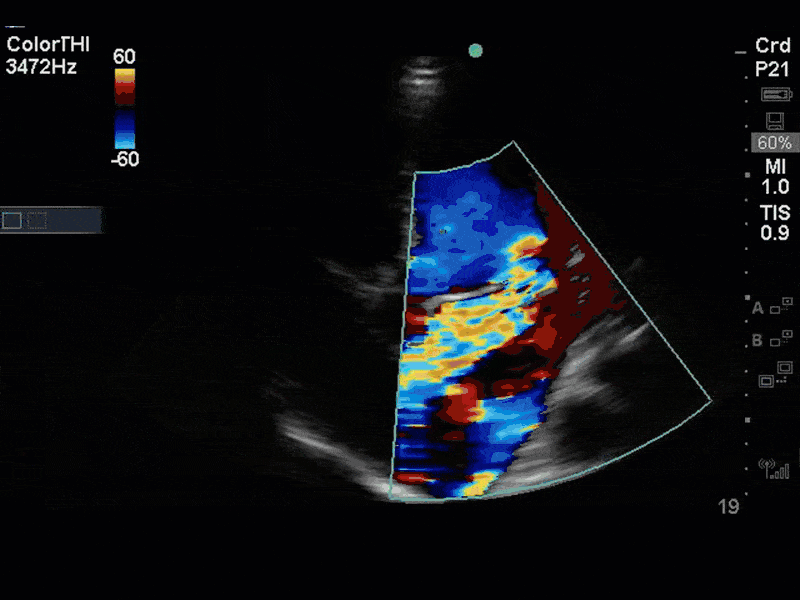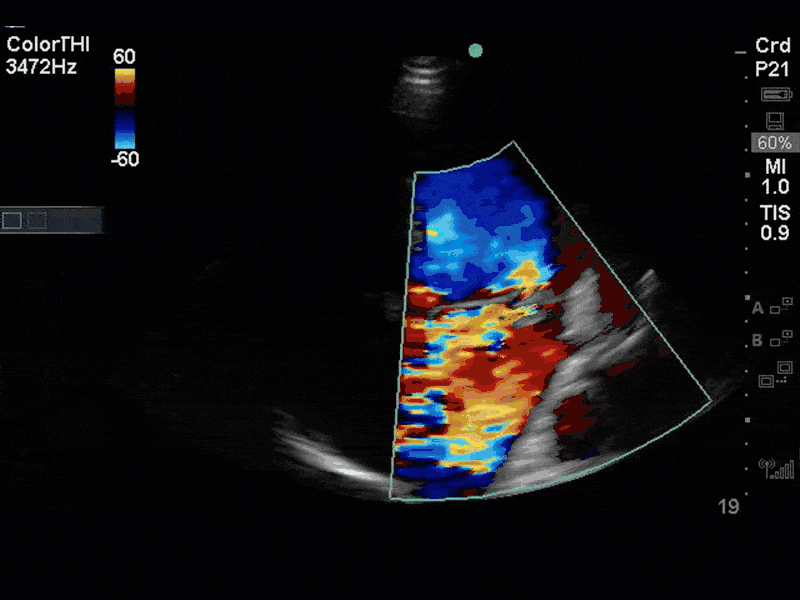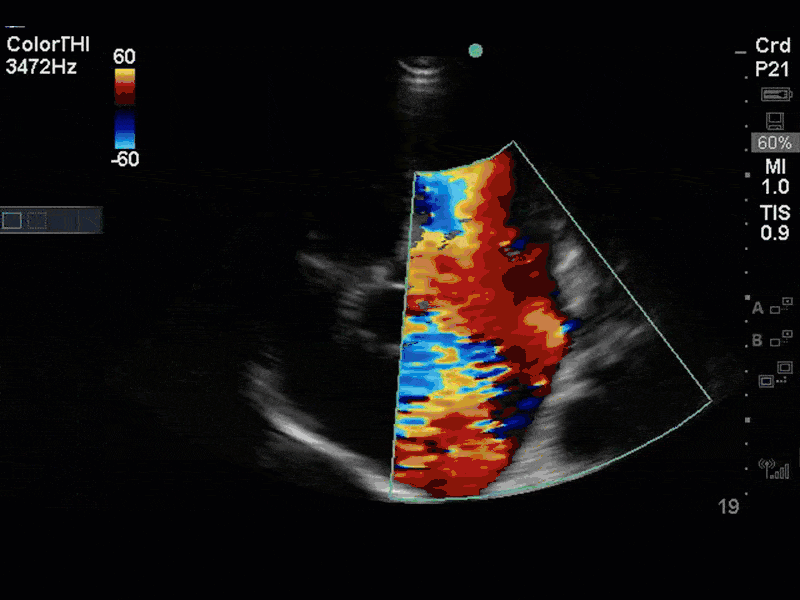
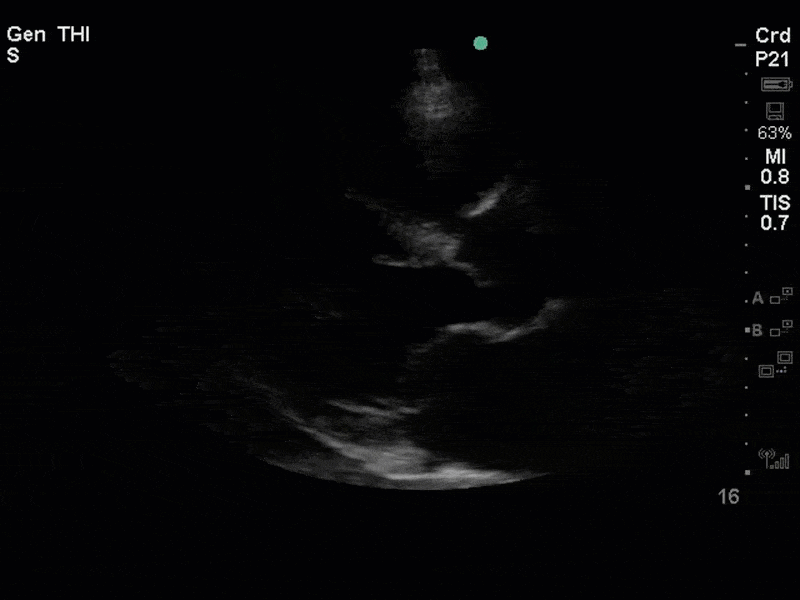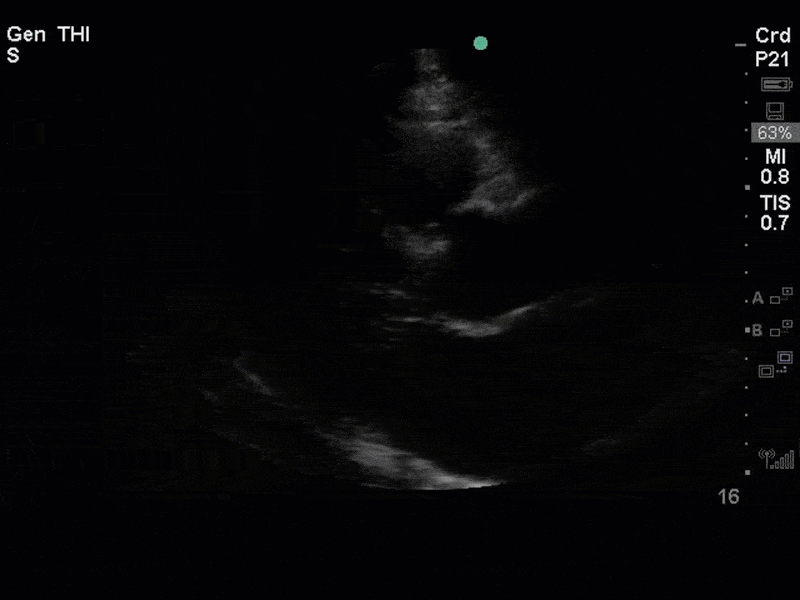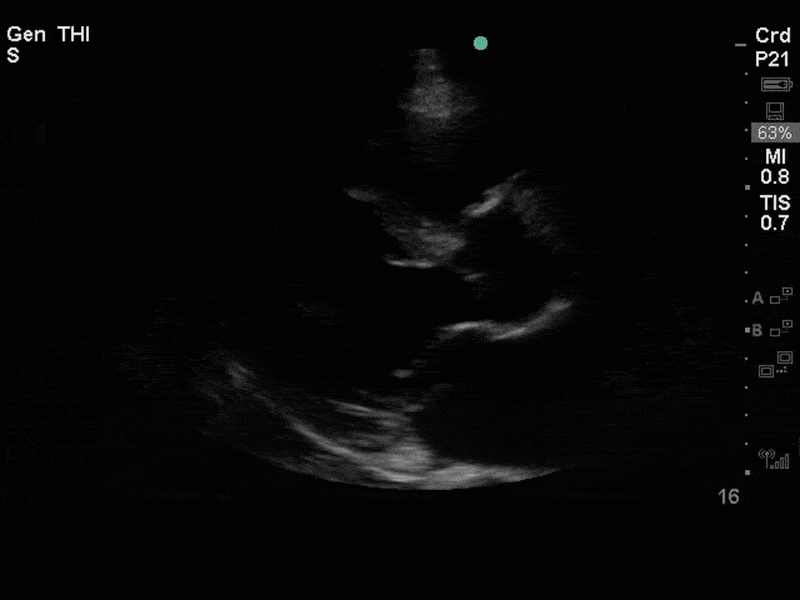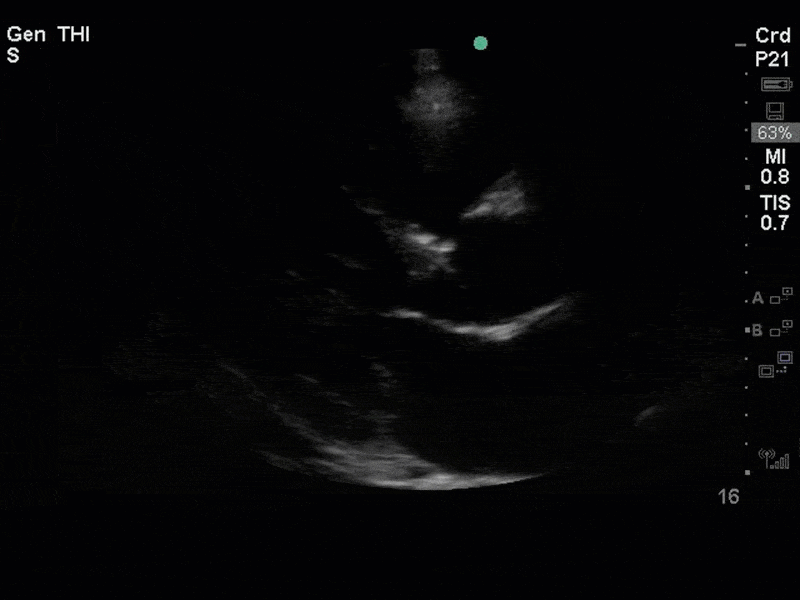
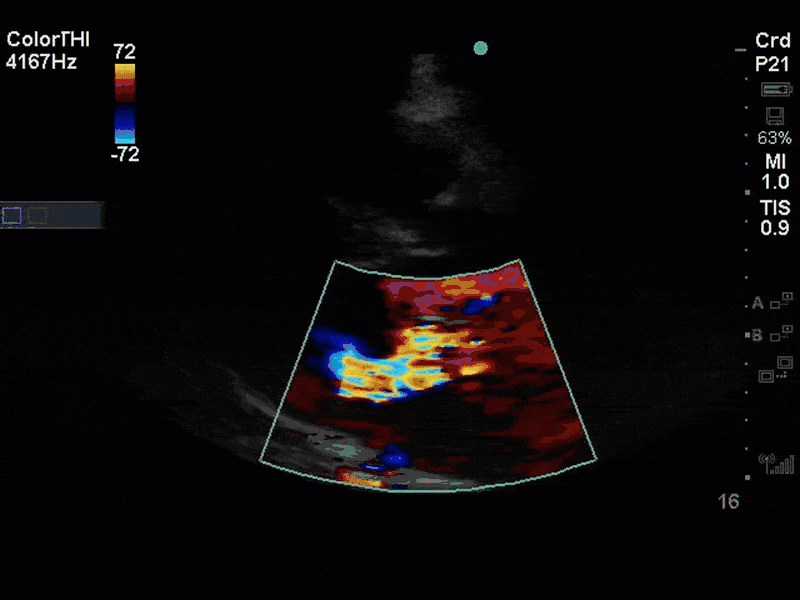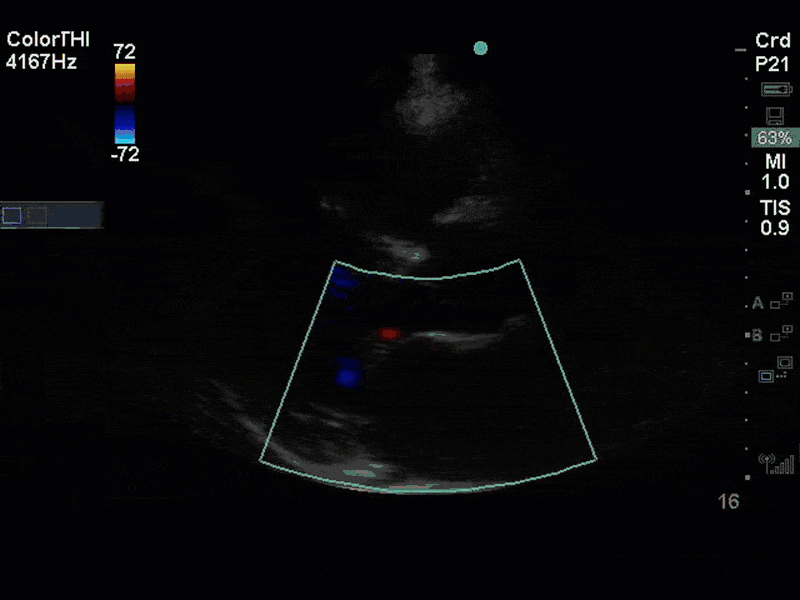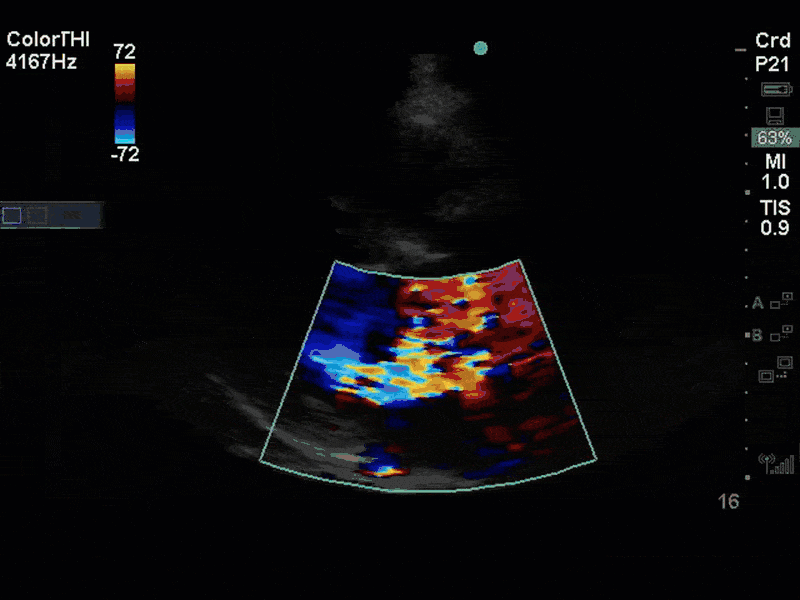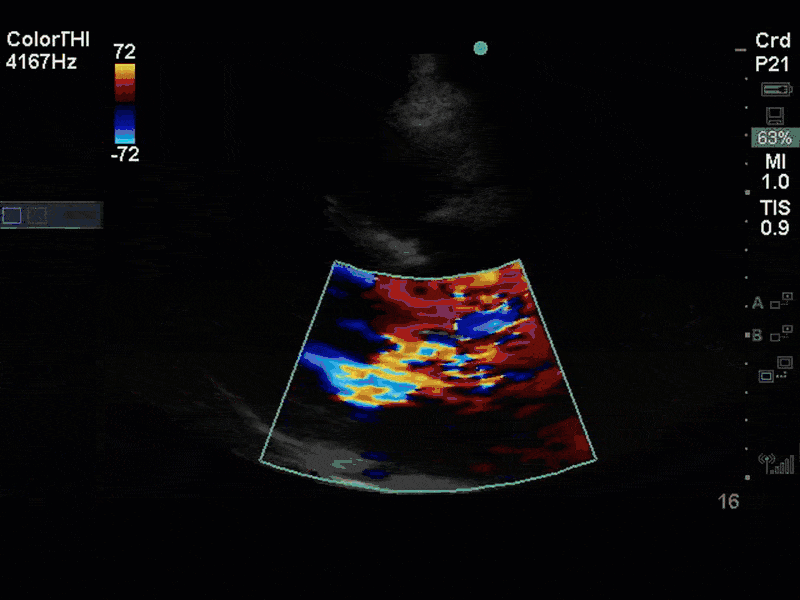
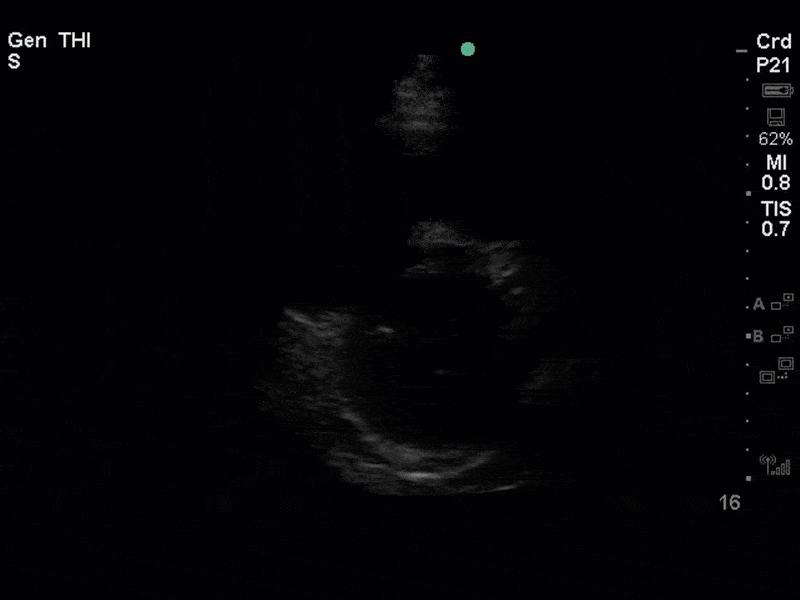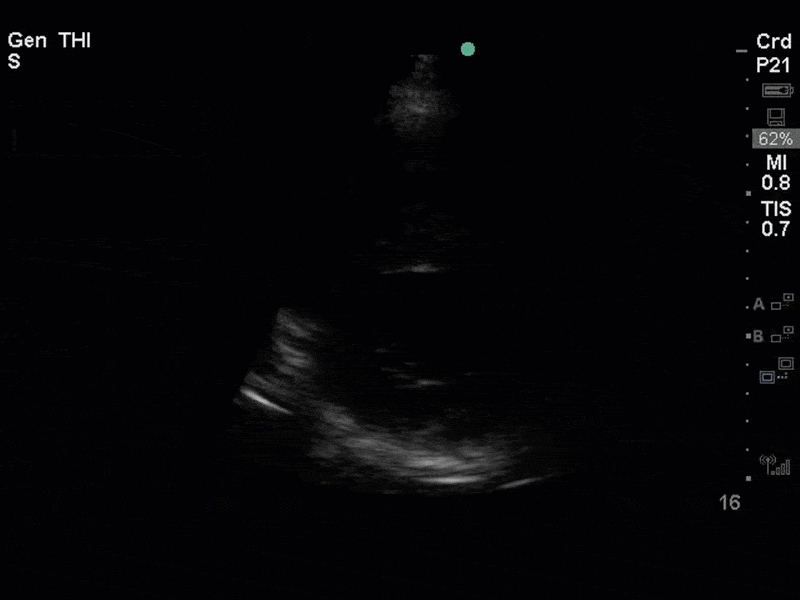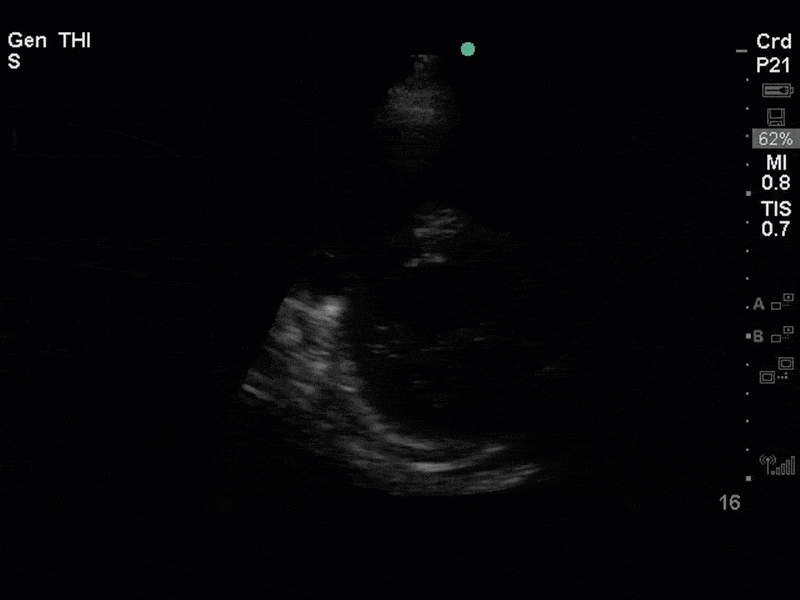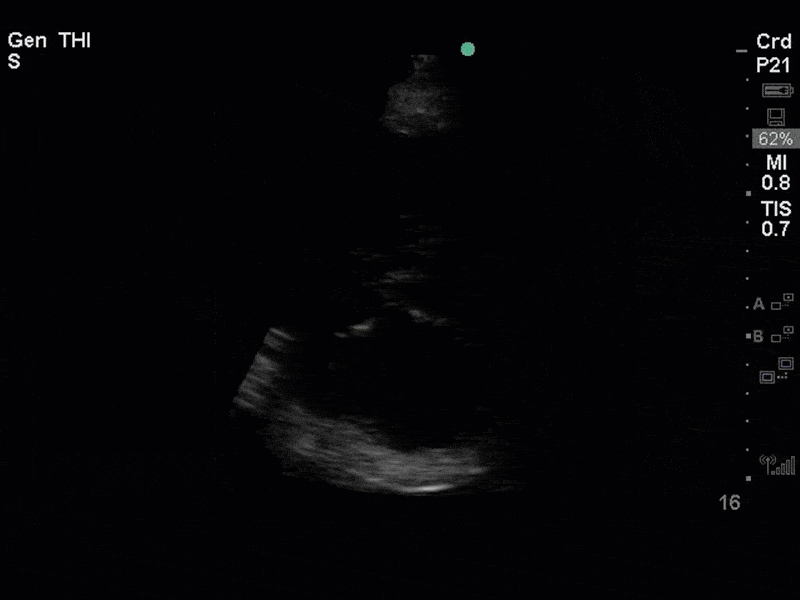
There is no clear definite lesion suggestive of endocarditis, but the images show a flail posterior mitral valve leaflet (PMVL) with associated severe MR. In the A4C view you can clearly see the abnormal mitral valve coaptation line, with the tip of the PMVL pointing towards the left atrium during systole (a hallmark finding of a flail leaflet). Colour doppler shows an eccentric, anteriorly directed MR jet.
Although, there was no obvious new vegetation on echocardiography (including a subsequent TEE) this patient met criteria (Duke criteria) for infective endocarditis. This is based on the patient fulfilling the major criteria of MSSA bacteremia, along with the presence her pre-existing MV pathology, fever, and evidence of septic emboli on her CT Head.
The flail leaflet had been documented previously secondary to myxomatous degeneration of the mitral valve apparatus with subsequent rupture of the chordae tendinae. The patient was actually awaiting open surgical repair of this valve, but unfortunately developed this illness prior to her operation. Overall, this case highlights a few important points about mitral regurgitation worth talking about.
First, is the general classification of mitral regurgitation. Mitral regurgitation can be classified as either primary or secondary. In primary MR the pathology is intrinsic to the valve itself. In contrast, secondary MR is a result of diseases of the LV (e.g. ischemic cardiomyopathy) and results from dilation of the MV annulus. The most common cause of primary MR is myxomatous degeneration causing mitral valve prolapse which can further progress to a flail leaflet, as seen in this case. Other causes of primary MR can include endocarditis, calcific leaflet degeneration and congenital abnormalities.
A variety of colour doppler, pulse wave doppler and continuous wave doppler techniques can be deployed to help grade the severity of MR. However, it is important to note that grading the severity of MR can be extremely difficult and nuanced, and as such, is often best left to the domain of formal echocardiography. In this case, the abnormal morphology of the MV (the flail leaflet) is consistent with severe MR, without necessarily having to apply more advanced Doppler techniques. Furthermore, the eccentric anteriorly directed jet is also a clue towards primary MV pathology, as secondary MR jets tend to be more central in nature.
The most important thing in this case would be to recognize the grossly abnormal 2D morphology of the MV and know to escalate this to a more detailed assessment. For those super keen on learning more about detailed MV assessment, you can check out the latest ASE guidelines on assessment of regurgitant lesions (attached below).