Case of the Week: December 9, 2019
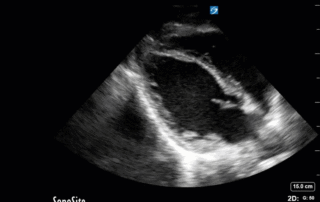
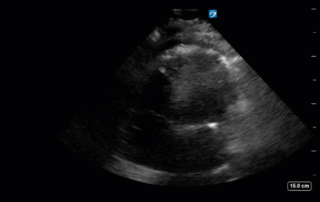
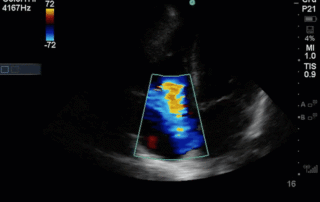
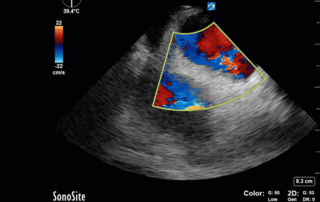
This week's case is a 67-year old woman who presented for an outpatient EGD. Post-procedurally she became hypoxic, so was brought to the ICU for monitoring and NIPPV. She was initially hemodynamically stable; however, over the next 6 hours she became profoundly hypotensive requiring very high doses of multiple vasoactive agents. She had a PMHx significant for severe COPD and HFpEF, with an Echo from earlier this year showing an EF of 50%.Below are her the clips taken upon arrival of the POCUS team the next morning. What do you think is causing her shock based on these images? You might want to make yourself comfortable, cause this week's case is a doozy and has a lot to unpack.*Note: given her marked hyperinflation she had no obtainable traditional parasternal or apical windows, so all views were obtained from a modified subxiphoid position (hence the unconventional axis). These scans are a good lesson, however, that you can still get lots of important information even when your views aren't perfect!
Case of the Week: December 4, 2019
85 yo M polytrauma from a high-speed MVC. Now recovering in the ICU, still intubated, but over the last few days has had worsening oliguric AKI and is now on 10mcg/min of NE. The POCUS team was asked to perform a “volume status” assessment. This is one of the most common requests we get. Below is a representative look at a typical set of images we try to acquire to help answer the million-dollar question of whether a patient would benefit from fluids. Have a look at the images below (which, be forewarned, are quite Doppler heavy) and see what you think!
Case of the Week: November 25, 2019
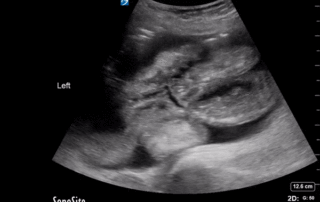
This week's COTW is a two-part special. This is a 70-year old man who presented with several days of diarrhea. Firstly, here are his abdominal images. What can you conclude based on these clips?
Case of the Week: November 20, 2019
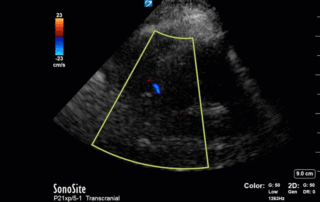
This is a case of a 52 yo F trauma patient with severe traumatic brain injury. She was intubated and transferred to the ICU where, given the severity of her TBI, an intraparenchymal ICP monitor was placed by neurosurgery. The ICP monitor was initially showing an ICP of 10. Overnight, however, despite no apparent clinical change, the ICP waveform was inconsistent and the readings were now showing values around 40-50. We thus performed a point-of-care TCD to help determine whether her ICP was truly elevated or whether the ICP monitor was giving spurious information. Have a look at the following images. Do you think the TCD spectral waveform is consistent with markedly elevated ICP?
Case of the Week: November 11, 2019
This is a 40-year old man status post-liver transplant (several months prior) who has had a complicated hospital course. He is now re-admitted with presumed septic shock (query HAP) and has been intubated for respiratory failure. He's also had a formal abdominal ultrasound commenting on periportal hepatic edema and signs of congestion.Based on the images below what interventions might you make to the team in addition to antimicrobial therapy? The team is particularly worried about right heart failure and elevated right-sided pressures - what do you tell them based on your findings?
Case of the Week: November 7, 2019
This is a 54 yo M who presented with acute hypoxic respiratory failure necessitating intubation and ICU admission. Post-intubation he had a P/F ratio of 54 despite a relatively unremarkable CXR. The PEEP was increased to try to improve oxygenation. A CTPA was ordered which was negative for PE and showed just a small right lower lobe consolidation. Given that the refractory hypoxia seemed discordant with the pulmonary pathology, concern was raised for an intracardiac shunt. A point-of-care TEE was performed including a bubble study. Have a look at the selected clips below and see what you think!