Advanced Critical Care Ultrasound Quantitative Assessment Resource
Our previous Critical Care Ultrasound Fellow, Marko Balan MD FRCPC, [...]
Case of the Week: February 14, 2020
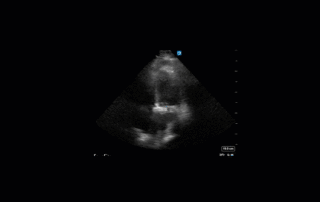
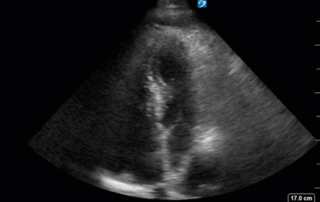
This is a 58yo F with ESRD with a history of known infective endocarditis of her AV for which she had previously completed a prolonged course of IV antibiotics. She was admitted to the ICU for worsening dyspnea. The POCUS team performed cardiac exam with some of the most striking clips shown below. What do you think? What complication of her endocarditis is shown and how would you grade its severity?
Case of the Week: February 6, 2020
This was a case of an 80 yo M, previously healthy, with no known significant previous medical history. He presented to the ED with acute decreased level of consciousness. The leading concern was acute spontaneous ICH. He was intubated and taken for a CT Head which surprisingly was completely normal. He was subsequently transferred to the ICU with the diagnosis of altered LOC NYD. A POCUS study was performed, and several cardiac clips are shown below. What do you think? Does this give a potential clue to what could be going on?
Case of the Week: January 29, 2020
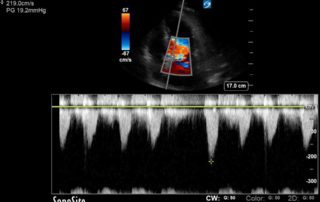
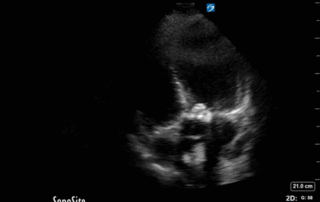
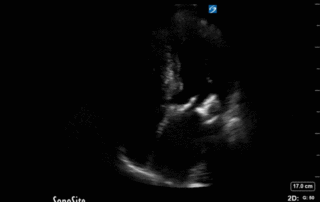
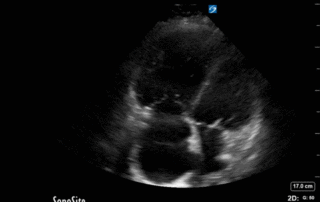
This is 65 yo M who presented with acute hypotension, hypoxia, and worsening AKI in the setting of known severe pulmonary hypertension secondary to a previous PE (CTEPH). He was admitted to the ICU for consideration of CRRT and IV flolan. A few days into his admission, the team asked for a POCUS cardiac assessment to reassess the status of his RV. Have a look the images below. Specifically, what do you think about the tricuspid regurgitation and estimated RVSP?
Case of the Week: January 22, 2020
This is a 74yo F with a past medical history significant for ESRD and severe PVD who was transferred to the ICU overnight with presumed septic shock thought to be related to left foot osteomyelitis. She had presented to the ED with refractory hypotension and altered LOC necessitating intubation and high dose vasopressors. The POCUS team went to do a focused cardiac exam, primarily to see if there was a cardiogenic component to his shock. The following TTE images were taken and the decision was made to perform a point-of-care TEE. What do you think is going on?
Case of the Week: December 18, 2019
This is a 70yo F with a recent diagnosis of left sided lung cancer. She presented with hemoptysis and was subsequently admitted to the ICU for monitoring. There she was found to be tachycardic at 120bpm and had reduced urine output. The patient had no known cardiac history and no previous echocardiogram on file. The POCUS team performed a focused echocardiogram, given that she was a newly admitted patient with ongoing tachycardia.