Case of the Week: November 7, 2019
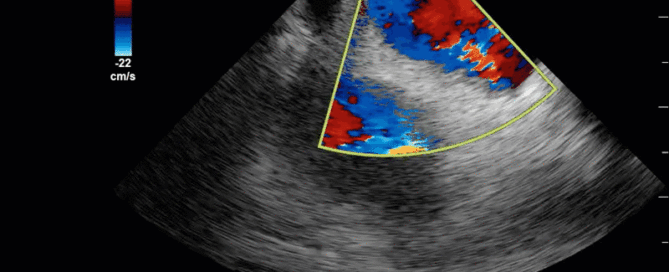
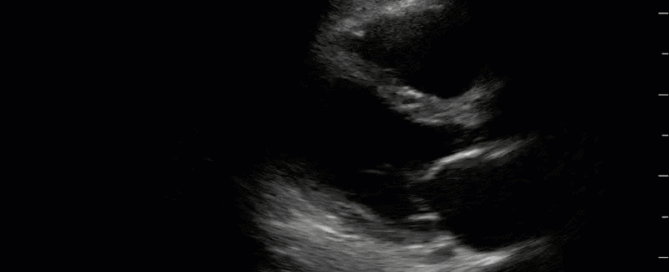
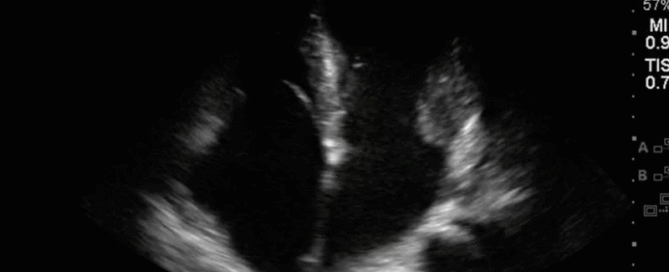
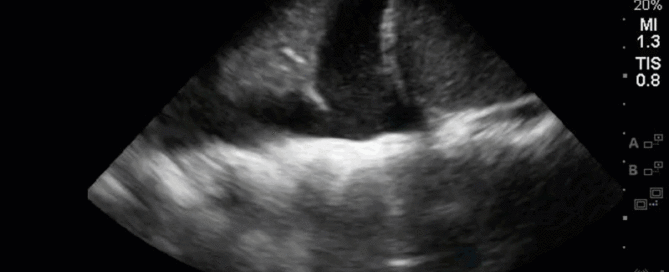
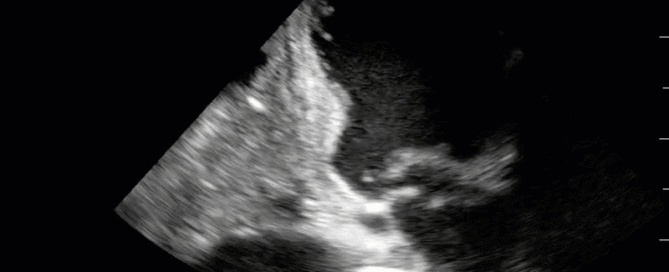
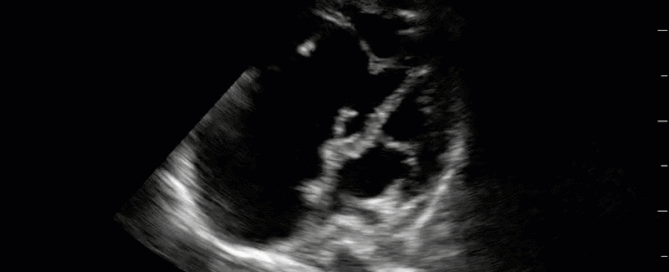
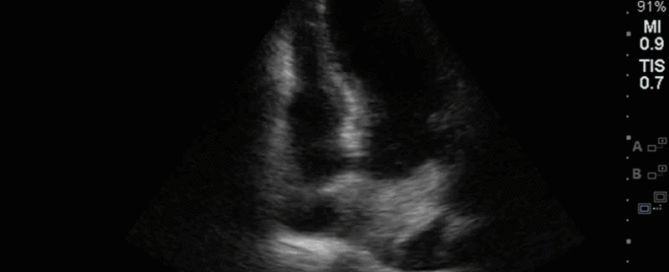
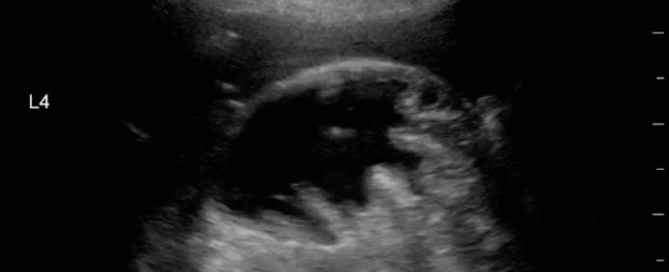
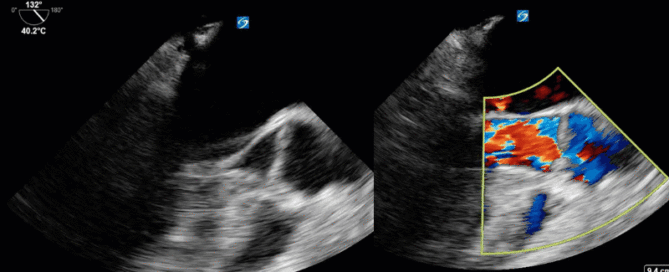
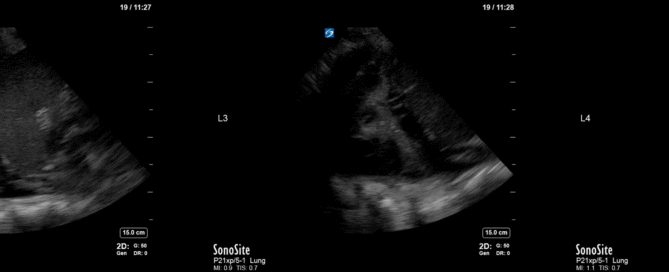
This is a 54 yo M who presented with acute hypoxic respiratory failure necessitating intubation and ICU admission. Post-intubation he had a P/F ratio of 54 despite a relatively unremarkable CXR. The PEEP was increased to try to improve oxygenation. A CTPA was ordered which was negative for PE and showed just a small right lower lobe consolidation. Given that the refractory hypoxia seemed discordant with the pulmonary pathology, concern was raised for an intracardiac shunt. A point-of-care TEE was performed including a bubble study. Have a look at the selected clips below and see what you think!