A Decade of Ultrasound: CRUS 2019
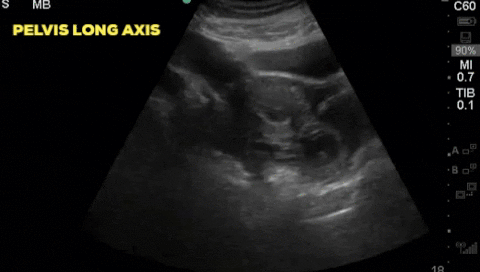
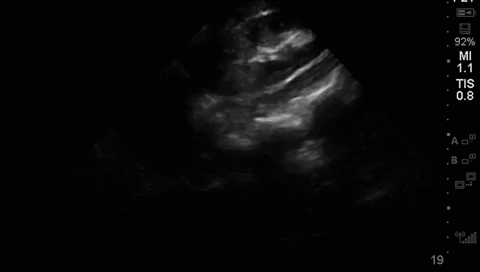
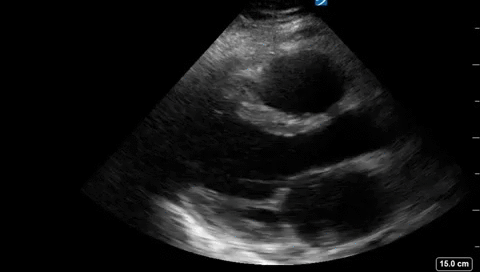
This year marked the 10th anniverary for the annual Canadian Resuscitative Ultrasound (CRUS) Course at Western University. Hosted at the sophisticated CSTAR (Canadian Surgical Technologies & Advanced Robotics) facility, the CRUS course drew trainees from across Canada to teach concepts in point-of-care ultrasound for use in the acutely ill patients typically seen in the ICU, the ED or OR. Participants engaged in didactic and hands-on [...]